Our views about the medicine practiced at Rome from the second century bce until the collapse of the empire in the seventh century ce are heavily influenced by the medical writings that survived to modern times. Additional information about the profession from an empire-wide perspective and the healing methods employed throughout the Mediterranean world can be drawn from a variety of other sources. There are accounts of illnesses in non-medical writers; the inscriptions medici and medicae placed on their tombs in the Latin-speaking west, or iatroi and iatrinai in the Greek-speaking east; the papyri of medical content from the dry sands of the province of Egypt which provide a glimpse of medical literature otherwise lost; amulets and charms that claimed healing properties which have been found throughout the empire. Nonetheless, the writers, such as the Greeks Soranus of Ephesus and Galen of Pergamum, both of whom journeyed from towns whose ruins still grace the coast of modern Turkey to practice at Rome, tell us much, and Greek names dominate among medical professionals and other healers, not only in the city and eastern provinces, but even in western ones (Korpela 1987; Nutton 2004, 164-6). Latin writers are not totally absent, but their own texts reveal the great extent to which doctoring among Romans had absorbed and assimilated the Greek antecedents. Two authors of the Julio-Claudian period, Aulus Cornelius Celsus and Scribonius Largus, will be investigated here in some detail together with Soranus and Galen.
In the reign of the emperor Tiberius (14-37 ce) Cornelius Celsus wrote a Latin encyclopedia on the four Artes, agriculture, military science, rhetoric, and medicine (Quint. Inst. 12.11.24). Only the seven-book ‘‘On medicine’’ (De medicina) survives to our time, and this work went virtually unmentioned after the late first century ce, although it was copied a number of times in the ninth and tenth centuries ce, thus testifying to continued interest by some in Celsus’ text; when these manuscript copies were rediscovered in the early fifteenth century, they created quite a stir (Reeve 1986a: 46-7). Celsus was remarkably knowledgeable about Greek secular medicine up to his own day, giving mostly favorable mentions to many of the important practitioners, such as Hippocrates in the world of Classical Greece, the anatomists Erasistratus and Herophilus in Ptolemaic Alexandria, and among those Greeks who made a reputation for themselves at Rome, Meges and Aesclepiades of Bithynia. Never once, however, did Celsus identify himself as a member of the medical profession, nor did he claim that he practiced medicine, although he did at times refer to visits he made to the ill and injured, the weak and dying (Nutton 2004: 1667; von Staden 1996: 401). Celsus’ stance was not that of a professional, but closer to that of a Cato, in that he was an educated Roman whom necessity compelled to acquire broad technical knowledge in many fields of human endeavor. He learned medicine to advise members of his household and those within his circle of his friends on how to preserve their health, or at least how to regain it if they should fall ill (Med. 3.4.9-10). His medical studies enabled Celsus to explain his own medical preferences in order to aid other paters familias in establishing their strategies for health care within their own households, and he passed judgment on what Greeks had said over generations concerning foodstuffs, therapies and drugs, and surgeries. His concern was to point out the more efficacious among the multitude of medical choices then available at Rome. For example, when examining maladies that afflict specific body parts and offering remedies, he noted with regard to diarrhea that Asclepiades of Bithynia had defied earlier authorities when he advocated drinks as cold as possible to ameliorate loose bowels, concluding with the observation, ‘‘Yet I myself think that each person should trust himself as to whether or not he should use a hot drink or a cold one’’ (Med. 4.26.4). The story that this same Asclepiades was famous for once having encountered a funeral procession conveying for burial a man still alive impelled Celsus to assert that medicine was a kind of educated guesswork (ars coniecturalis) in which experienced practitioners, although not immune to deceptive symptoms and wrong guesses, were nonetheless to be relied upon in most instances, more often able to benefit the sick than not (Med. 2.6.13-18). Celsus also found room in his survey for therapies drawn from folk traditions. After listing doctors’ remedies for toothache, including extraction, he finished off with a therapy developed by country people that involved a steam bath with an herb from the mint family (mentastrum), roots and all, for this not only caused profuse sweating and a flow of phlegm from the mouth, but ‘‘ensured good health for a year or longer’’ (Med. 6.9.7). Professional medical men may have been embarrassed when abscesses in the lymphatic glands called strymata recurred after treatment, but Celsus again interjected the experience of country-folk who cured these by eating a snake (Med. 5.28.7b). Some even freed themselves from epilepsy (for which disease Celsus employed the Latin term morbus comitialis) by drinking the blood of a gladiator whose throat had been cut ( Med. 3.23.7), a remedy also recorded by Pliny (Nat. 28.2.4).
Celsus underscored in his preface the fact that it was men who led their lives in luxury and indolence that required elaborate doctoring: ‘‘This happened first among the Greeks and then later among us Romans’’ (Med. praef. 4-6). He also began his text proper by reiterating that the man in good health of body and mind had no need for doctors, while the weak did, for these latter were, for the most part, modern city-dwellers immersed in literary pursuits (Med. 1.1-1.2). Pliny shared Celsus’ dream of a bygone Golden Age of healthy and hearty Romans, free of Greek doctors, and Pliny’s boast that few Romans practiced medicine alone of the Greek arts, despite the great profits to be had (Nat. 29.8.17), seems born out not only by the predominance of Greek names among medical practitioners known to have doctored at Rome, as well as by Celsus’ own On Medicine (Nutton 2004: 164-6). On the one hand, there is much Greek medicine in Celsus’ text, for he easily included Greek words for diseases, bodily parts, therapeutic agents, and surgical instruments into his Latin narrative, explicitly identifying them as such on nearly 200 occasions (von Staden 1996: 394-6). When his description of bodily parts and their ailments descended down from the head to the male genitalia, he emphasized the appropriateness of Greek words for anatomical parts, for these were everywhere met and were not only preferable to the coarseness of Latin’s sexual vocabulary, but they enabled patients to discuss more freely a complaint such as a swollen penis (Med. 6.18.1). Yet Celsus made clear that the educated Roman should be discriminating in his use of Greek medicine, maintaining his health and vigor through the hard work of sailing, hunting, and attending to matters on his country estates, as was the Roman way. Celsus’ aim was to record, evaluate, and arrange for Roman use what Greek medical writers had produced. Still his careful compendium never circulated as widely as Pliny’s Natural History, and medical excerpts from the latter’s more garrulous work remained particularly popular (L. D. Reynolds 1986b: 309-16; Reeve 1986b: 352-3).
Scribonius Largus was, by contrast, a medical professional and he accompanied the emperor Claudius to Britain in 43 ce, perhaps as private physician to a member of the emperor’s entourage, since Claudius’ personal physician was a Greek from the island of Cos, Gaius Stertinius Xenophon. Largus was well known in the imperial household, for he not only dedicated his Latin work on drugs ( Compositiones) to Gaius Julius Callistus, one of Claudius’ most trusted freedmen, but he also included recipes for medicaments employed by members of the Julio-Claudian family, such as a restorative salve used by Augustus’ wife Livia and the younger Antonia (mother of Claudius) that countered arthritic pain and, when rubbed on joints, made them warm and supple (Comp. 271, 268). Largus wrote his drug book after his return from Britain, dividing it into three sections: medicaments for diseases in a ‘‘head-to-toe’’ arrangement, from headache to gout; theriac remedies for insect stings, snake bites, and antidotes for poisons; and a final section on plasters, many ofthem named for the Greek surgeons who invented or popularized them. Largus was apparently born in Sicily and trained there before moving to Rome, for his teacher was from the Sicilian town of Centuripae. In addition, Largus occasionally mentioned medical practices of the island, noting, for example, that the pointed trefoil grew in plentiful quantities in Sicily, but not elsewhere, despite its usefulness against snakebites; he first recorded the Latin name of the plant (trifolium acutum) and then the Greek (oxytriphyllon, Comp. 94, 163). As a native of Sicily, he was most likely bilingual, and some 22 of his recipes were quoted in Greek by Galen in his own drug books, suggesting that Largus himself may have written a now lost Greek version in addition to the Latin drug book we now have (Sconocchia 1983). Largus’ Latin version served as basis for the pharmaceutical treatise by Marcellus of Bordeaux at the end of the fourth century CE, now expanded with remedies from Marcellus’ native Gaul. A printed text of Largus’ Compositiones was produced in Paris in 1529, but the manuscript used for that edition soon disappeared, and only in the latter decades of the twentieth century has a manuscript of the Compositiones, copied at the beginning of the sixteenth century, been discovered in the library of the cathedral of Toledo, Spain (Reeve 1986b: 352-3).
Like Celsus, Largus often glossed names for diseases and medicinal plants with their Greek names, underscoring once again the extent to which Greek medicine had become naturalized in a Roman setting. He likewise shared Celsus’ interest in popular remedies, including a therapeutic recipe for epilepsy ( morbus comitalis), advocated by a certain Roman lady, that required fresh blood from a male turtle or a male dove if the patient were a boy, but from the female, if a girl. Largus looked with distaste, however, upon remedies in which epileptics were ordered to drink blood from their own veins or eat bites from the liver of a dead gladiator, declaring such practices outside the professional practice of medicine ( Comp. 17). Largus’ elaborate dedicatory letter to Callistus began with the much-quoted statement by the Alexandrian Herophilus that medicaments were ‘‘the hands of the gods’’ (Comp. praef. 1; von Staden 1989: 416-18). ‘‘And a reasonable view, in my opinion,’’ Largus went on, ‘‘for the healing which divine touch brings about, medicaments long in use and tested can also effect.’’ He went on to argue that remedies from plants and their roots were the oldest branch of medicine, because the race of men was essentially cowardly and did not willingly undergo the healing that involved cutting or cautery. Largus chastised those doctors who eschewed pharmacy, for they were violating the promise medicine declared in its oath - that it would come to the aid of all who asked for help on an equal basis and never bring harm to anyone, not even giving an evil medicament to one’s foreign enemies. Not only do these statements make clear that Largus viewed doctors as moral men, bound by a common code of ethics, but he was paraphrasing for the first time from our point of view portions of what we refer to as the Hippocratic Oath:
Hippocrates, the founder of our profession gave us the beginnings of our endeavors through that Oath in which one promises not to give a medicament to a pregnant woman that will expel her fetus. Each doctor must make this clear to his students, shaping their minds from the outset toward the good of mankind. Anyone who thought it criminal to damage the precarious hope for a human being before its birth is certain to judge it all the more criminal to harm the living. Hippocrates therefore considered it of great importance that each doctor preserve the reputation and honor of medicine with his spirit pious and holy, conducting himself in accordance with his precept that medicine is a science of healing, not of destroying. (Comp. praef. 5)
Appealing to the fifth-century bce Greek doctor Hippocrates of Cos as an authority figure in medical matters became increasingly common during the Hellenistic period, and by the time of both Celsus and Largus he had been accepted at Rome as the ‘‘Father of Medicine.’’ About two generations after Largus, Soranus of Ephesus, then practicing at Rome, also discussed the prescribing of abortives and contraceptives ( Gyn. 1.60-5). Because nothing was known about the ovulatory cycle or the early events in pregnancy, Soranus repeated the kind of advice most medical writers gave throughout antiquity, yet by no means the advice a modern gynecologist would give. Namely, that fruitful intercourse, designed to result in conception, should take place as menstruation was abating and an appetite for coitus present (Gyn. 1.43-5). Soranus thought it better for a woman who did not want to conceive to take contraceptive precautions and he advised such measures as holding her breath and drawing back a bit as the man ejaculated, so that his generating seed not be thrust too deeply into her uterus; a douche after intercourse might also be useful, or a forceful sneeze. Soranus’ prescriptions for precoital insertions with contraceptive intent included ingredients that were styptic, clogging, and cooling, so as to make the os uteri close before intercourse took place. He listed other contraceptive remedies that were more potent and, in his view, potentially dangerous, since they not only irritated the interior of the uterus, but destroyed a fetus, if one had already been conceived (Gyn. 1.60-5). Soranus knew two abortive methods; the phthorion destroyed a fetus through drugs and the ekbolion expelled the fetus through shaking and leaping. When Soranus explained his practice with regard to abortion, he too quoted the Oath, ‘‘I will give no one an abortive,’’ adding that it was medicine’s task to protect what nature engendered, but he also turned to another treatise in the multi-authored Hippocratic Corpus, ‘‘Nature of the Child,’’ for here the medical writer counseled a pregnant flute-girl, a slave who belonged to one of his household, to leap into the air and kick her buttocks with her heels (Hippoc. Nat. puer. 13). On her seventh leap the conceptus fell out with a plop, and the girl stared at it in surprise. From this latter example that Soranus also attributed to the ‘‘Father of Medicine,’’ he concluded that abortion was advisable if allowing a pregnancy to proceed to term endangered the mother’s life, especially if she were too young and her uterus underdeveloped. Soranus refused, however, to prescribe abortives if the motive were to hide an adulterous affair or to preserve youthful beauty. Both the prostitute and the adulteress may well have looked to abortive techniques as a way out of inconvenient pregnancies (Kapparis 2002: 97-120). By contrast, married couples worried about their ability to leave behind them two adult children as replacements at parents’ deaths, because the levels of infant mortality were high. Wives in the Roman world appear to have given birth throughout their fertile lives, rather than deliberately restricting their childbearing years primarily through contraceptive procedures, as is currently done in developed countries of the West (Frier 1994). Prolonged nursing of an infant by the mother for two or three years, as was the habit in the Roman world, did have a dampening effect on the mother’s fertility, and for those who wished to conceive again Soranus advised the employment of a wet nurse. Even better, he thought, was to have several wet nurses available to suckle the child, lest a single wet nurse become ill or die (Gyn. 2.19-20).
Soranus practiced his medicine in accordance with the principles of Methodist physicians who concentrated on treatment and eschewed theorizing about unseen happenings inside the human body, or worrying overmuch about the kind of imbalance in bodily humors causing an illness. It did not matter to Methodists whether the patient’s body contained a dearth or surplus of a particular bodily fluid, such as phlegm and black or yellow bile; rather they simply investigated whether the body was too constricted, as in constipation, or too relaxed, as in diarrhea, and set about rectifying the state of the patient’s body in order to return it to health. This medical approach appealed to Romans, and the sect remained popular into late antiquity, especially in the provinces of North Africa. Soranus’ Gynecology is his only treatise to survive to modern times in Greek, and it did so in a single copy made in the thirteenth century. In the fifth century CE Caelius Aurelianus, a Methodist of African birth, produced Latin translations of Soranus’ On Chronic Diseases, On Acute Diseases, and also his Gynecology; these were read and revised throughout the earlier Middle Ages, until superseded at the beginning of the thirteenth century by medical texts being produced at the new medical center of Salerno (Hanson and Green 1994: 1045-61).
Galen of Pergamum spent the majority of his long adult career in Rome, doctoring, philosophizing, and climbing the city’s social ladder to become one of the physicians who regularly attended the emperors and the imperial household - from Marcus Aurelius to Septimius Severus (161-c.216 ce). In his medical autobiography Prognosis Galen took great pleasure in recounting the night he was summoned to sleep at the imperial palace and successfully diagnosed that the emperor’s current ailment was only an upset stomach, due to the cold food he ate for lunch that caused a flow of phlegm into his stomach. Thus this was not the attack of fever the emperor feared, and, according to Galen, Marcus Aurelius responded to the diagnosis by asserting, ‘‘We have one doctor, and he is a consummate gentleman.’’ Galen then claimed, ‘‘He was always speaking of me as the first among physicians and the only genuine philosopher’’ (Praecog. 11). As a Methodist, Soranus paid scant attention to bodily humors, and, while Celsus occasionally mentioned a superfluity of phlegm and bile as disease agents, he did so in a way reminiscent of many Hippocratic writers, with phlegm predominant in diseases afflicting the eyes and head, but black bile, ‘‘which the Greeks called melancholia,” appearing not only in cases of ophthalmia, but in abscesses all over the body (Med. 2.1.6). It was Galen who set the four humors (phlegm, yellow bile, black bile, blood) into prominence in physiology and nosology, and although he asserted that this was what Hippocrates had done, it was principally the treatise ‘‘Nature of Man’’ within the Hippocratic Corpus that likewise insisted on these four particular fluids. The four humors and the four qualities (hot/cold and wet/dry) served as organizing principles for Galen’s classifications of foodstuffs, for some foods were heating, others cooling, moistening, or drying, in various degrees; some made the humors thicker, others thinned them. Phlegm was more likely to dominate the body in winter, blood in summer, with the biles relegated to fall and spring. The humoral theory, as formulated by Galen, remained central in physiology and nosology for more than a millennium and a half thereafter, and the four resulting temperaments for human beings - phlegmatic, bilious (or ‘‘choleric’’), melancholic, and sanguine - were, for example, one shorthand means Shakespeare used to sum up the personalities of his characters.
Galen not only considered Hippocrates the greatest of medical authorities, repeatedly citing him, but his picture of Hippocrates as practicing physician and author of medical texts increasingly meshed with Galen’s own view of himself and his experiences to a degree not known elsewhere (Nutton 2004: 216-29; A. E. Hanson 1998a). Galen’s long active career of some 60 years, his strict work habits, and his intellectual restlessness resulted in a mammoth output of treatises on medical, philosophical, and linguistic topics. It has been estimated that his writings in Greek represent ten percent of all surviving Greek literature written before 360 ce and that he must have written or dictated to a scribe about two or three pages every day of his working life (Nutton 2004: 390). Determining the exact number of items in Galen's bibliography, however, is a complicated matter: towards the end of his life, Galen composed a descriptive catalog of what he had written, On His Own Books, and a companion volume, On the Order of His Own Books, explaining the order in which readers at varying degrees of medical sophistication, especially in anatomy, should approach them. Galen, however, neglected to mention a number of works he thought lost, and the ninth-century Arabic translator of Galen, Hunain ibn Ishaq, listed 50 works known to him in Baghdad that Galen had omitted from his catalogue. The standard edition of Galen’s works by C. G. Kuhn runs to some 16,000 pages, but in the nearly two centuries since it was printed in the 1830s, discoveries of works by Galen previously thought lost have been made, especially in translations into Arabic, Syriac, Armenian, Hebrew, or Latin, increasing the number of pages by at least one quarter (Nutton 2002: vii). Galen dominated the medicine of the Greek-speaking east for the next millennium, as the number of languages into which his works were translated makes clear. The breadth of his learning and his passion for anatomy resulted in a medical system whose conservative teleology appealed to learned men, pagan, Christian, and Muslim alike. With the revival of learning in the late Middle
Ages and throughout the Renaissance his writings were studied afresh, first through Latin translations from the Arabic and then through the Greek books that their owners carried with them from Constantinople to the west after the city’s capture in 1453. Galen’s enthusiasm for Hippocrates revived interest in the Hippocratic Corpus, and these texts also made their way back to Italy and the west.
Galen began his study of medicine at age 17, when Asclepius appeared to his father in a dream, urging him to add medicine to his son’s studies in philosophy, and for the next 11 years Galen journeyed around the eastern Mediterranean in pursuit of important teachers, training first in Pergamum and then at Smyrna, Corinth, and finally Alexandria. Little wonder, then, that Galen heaped scorn on Thessalus, a Methodist physician and contemporary of the emperor Nero (54-68 ce), who boasted he could teach medicine to his pupils in six months. Galen’s first professional appointment was as physician to the gladiatorial school at Pergamum, and from gladiators’ wounds and fractures he not only became skilled in practical surgery, but also acquired a fascination with anatomy and physiology. In his Examinations of the Best Physician, Galen drew attention to the fact that only two wounded gladiators died in his care, while 16 had perished at the hands of his predecessor (9.7).
Once arrived and established in Rome, Galen gave anatomical demonstrations for a time before crowds of invited guests; at one such session he demonstrated the mechanisms of speech by ligating nerves in the muscles of a pig’s larynx, disabling the animal’s ability to squeal (Praecog. 5). Galen continued to dissect and vivisect animal bodies, for the intellectual and moral climate of Rome had little tolerance for the opening of human bodies, as had once been the case for the anatomists of Alexandria in the mid-third century bce. Galen usually preferred to work with pigs, goats, or oxen, rather than apes, because one thus avoided seeing the unpleasant expression on the ape’s face when it was being vivisected and because demonstration of vocal apparatus worked better on animals with a loud cry, ‘‘a thing one does not find with apes’’ (Anat. admin. 9.11-15). In his Anatomical Procedures Galen described how to open the mid-section of a pregnant goat, revealing a fetus still contained in the womb; the discussion is impressive not only for its surgical skills, for the mother goat was stitched back up to live another day, but also for the demonstration that a fetal heart beat independently from the heart of the mother (12.4-6). Galen also corrected Herophilus’ mistaken analogy from male anatomy that a woman’s ovarian tubes implanted into the neck of her bladder, just as spermatic ducts did in men, noting instead that they grew from the ovaries into the body of the uterus (Sem. 2.1). Debates as to which organ was in control of the human body (hegemonikon) continued in Galen’s time, and, although he was convinced that it was the brain, others still argued for the heart. Galen, however, adopted the erroneous view from Hellenistic predecessors that there was a confluence of nerves and blood vessels at the base of the human brain which resembled layers of fishermen’s nets, the retiform plexus (or rete mirabile, as it came to be called), and, confident that this convoluted vascular structure existed in humans, he assigned it a physiological function important to him - that of transforming life-giving breath (vital pneuma) that flowed in the arteries into the animated breath (psychic pneuma) that activated the brain and nerves to govern both sensation and motion (Usupuls. 2, Anat. admin. 9.8; Rocca 2003: 202-19, 249-53). But the retiform plexus is not found in either humans or apes, but exists in mammals such as the ox, goat, or pig, animals Galen preferred to dissect and vivisect. What Galen said about cranial and cerebral anatomy is accurate for oxen. By the early sixteenth century some Renaissance anatomists were stating openly that they could not find the Galenic rete mirabile in the cadavers they dissected. For example, Berengario da Carpi (c.1460-c.1530), a lecturer at the flourishing medical center of Bologna, denied its anatomical existence in human bodies, but retained Galen’s physiology by transferring the function of the rete mirabile to the pial arteries; and despite his anti-Galenic rhetoric, based on an awareness that Galen’s anatomy derived for the most part from his dissections of animals, Andreas Vesalius (1514-64) nonetheless also reassigned Galen’s physiological functions for the rete mirabile to the cerebral arteries. Galen never anticipated the domination he would achieve over subsequent medicine, but threads of ambition and self-promotion run through his many writings, underscoring his hope that he would be recognized as having created a medical system which summarized and obviated the need for others to read his predecessors. His treatises survived intact the process of epitomization into the works of the Byzantine compendiasts, while those of his approximate contemporaries Archigenes, Rufus, and Philumenus did not.
The medical texts from antiquity we read today survive because they continued to be read century after century and were recopied by hand in sufficient numbers up to the time when the printing press was invented in the mid-fifteenth century. Thereafter, multiple copies of ancient physicians’ books became increasingly available to Renaissance readers. The writings of many, however, were early lost, and we know only their names from mentions in Celsus, Soranus, and Galen. Material objects from the Roman past afford us some notion of the medical personnel who functioned outside the city and hint at the medicine they were practicing. About 140 ce, a midwife named Scribonia Attice had an attractive brick tomb constructed for herself, her husband Marcus Ulpius Amerimnus, and members of their familia, both blood kin and freedmen, in the cemetery that lined a road leading out from Trajan’s newly built harbor for Rome at Portus (Isola Sacra, tomb #100). She had the tomb decorated with terracotta plaques: the one at right depicted Scribonia Attice herself, in attendance at a birth; she knelt in front of a birth chair on which the parturient sat and she held out her arms to receive the neonate, who would soon drop from her mother and through the perforated seat in the birth chair. The birth chair was slanted gently backwards, had handles for the parturient to grip, and an attendant behind to support her back, the very equipment and helper called for by Soranus (Gyn. 2.3.1-2) (Figure 25.1a). The plaque on the left shows that Scribonia Attice’s husband Amer-imnus was a surgeon; he was in the act of drawing blood from a patient’s leg, while various of his specialized instruments (scalpels of various sizes, hooks, and probes) lay spread out in the background (Figure 25.1b). Both husband and wife were of Greek origin, as their cognomina ( Attice and Amerinmos) and the name of Attice’s mother Callityche demonstrate, but their nomina (Scribonia and Ulpius) were thoroughly Roman, and the dedicatory inscription on their tomb was written in Latin. The couple was likely to have acquired their nomina when they were manumitted, with Amerimnus’ praenomen and nomen (Marcus Ulpius) implying that he was probably an imperial freedman of Trajan. Attice and Amerimnus took pride in their work as medical practitioners, for their skills enabled them to become full participants in the world in which only Roman citizens were legally privileged and socially advantaged. They themselves owned slaves, despite their servile origins, and had manumitted

Figure 25.1a Relief of Scribonia Attice assisting with a birth

Figure 25.1b Relief of Marcus Ulpius Amerimnus drawing blood some of them. It was nonetheless for their medical skills that they wished to be remembered in the cemetery of Isola Sacra, where many others also advertised the trades they practiced in life.
Elaborate collections of medical instruments ( instrumentaria) have been found all over the Roman Empire, as well as in Italy and the vicinity of Rome, consisting not
Only of scalpels, hooks, and probes, but also forceps of various design for specialized tasks, wound retractors, needles, and cupping vessels (Jackson 1988: 112-23; Jackson 2003). Many scalpels were finely crafted in different shapes, with blades of steel from the Alpine province of Noricum, and the assemblages unearthed from the towns of Pompeii and Herculaneum, destroyed by the eruption of Vesuvius in 79 ce, have provided particularly large and elegant examples (Bliquez 1994). Some instrumen-taria were buried with their owners, while others were excavated from the military hospitals (valetudinaria) that became an essential part of the permanent fortresses housing the legionary and auxiliary troops who guarded the edges of the empire. From the days of Julius Caesar’s wars in Gaul, special areas of a military camp were set aside in which wounded and ailing soldiers were cared for(BG 6.38), and well known are the hospital facilities later constructed in the forts of Britain and along the Rhine-Danube frontier. The wooden writing tablets that survive from the fort at Vindolanda adjacent to Hadrian’s Wall include an interim strength report for the auxiliaries in the First Cohort of Tungrians stationed there in the early second century ce, listing those away from the fort on army business (absentes) and those at the fort currently unfit for active service - the sick (aegri), the wounded (volnerati), and those with ophthalmic diseases (lippientes; Bowman and Thomas 1994, T. Vindol. 2.154). Similar strength reports are known from the First Veteran Cohort of Spaniards, stationed in the early second century in Moesia on the lower Danube; from the First Equestrian Cohort of Lusitanians, stationed in Egypt (dated to August 31, 156 ce); and from the Twentieth Cohort of Palmyrenes, stationed in the early third century at Dura-Europus on the middle Euphrates (Fink 1971, text nos. 63, 64, 8). The general public was not serviced by hospital facilities until the empire had become Christian and charity for the sick and dying was considered part of the Christian’s duty. Galen’s appointment as doctor to the Pergamene school of gladiators demonstrates, however, that specialized groups were likewise cared for; Galen noted that gladiators were wounded in ways similar to soldiers in the army and also ordinary people, especially hunters. In his commentary to the Hippocratic treatise ‘‘Fractures’’ he drew attention to the bandages and plasters he applied to patients’ wounds, always soaking the freshly stitched-up ones with dry, red wine (Hipp. Fract. comment. 3.21; cf. Comp. med. per gen. 2.17 and 3.9). Meticulous treatment of this nature would have lessened the likelihood of infection.
Papyri from the Roman province of Egypt likewise clarify other aspects of the medicine being practiced outside of Rome itself, for the desert sands preserved written texts of all kinds in great numbers. Galen boasted that his treatises were being read throughout the empire, and his claim was bolstered somewhat by finding a copy of his Opinions of Hippocrates and Plato in circulation in Egypt no later than a generation after his death, and perhaps even during his lifetime (A. E. Hanson 1985: 32-47). Illustrated herbals, describing the plants pictured and clarifying their medicinal properties, were popular in the province from the second century onwards (A. E. Hanson 2001: 585-604). Some of the earliest parchment codices to survive from late antiquity were also elegantly illustrated herbals - the Greek Materia medica by the mid-first-century ce pharmacologist Dioscorides of Anazarbus, which was copied and illustrated in or near Constantinople about 512 ce as a wedding present for an emperor’s daughter (MS Vindobonensis med. gr. 1), and, in the west, the Latin pseudo-Apuleian Herbarium (MS Leidenensis Voss. Lat. Q.9) copied later in the same century. Greek texts intended to provide summaries of medical information were also common in Egypt, sometimes as a list of medical definitions and sometimes in a question-and-answer format, and, like the herbals, they offered some degree of medical self help to the literate, as well as being tools in medical education. Much attention was paid in these texts to diseases of the eye, and while this may be due in part to the ancient medical habit of discussing diseases in a ‘‘head-to-toe’’ arrangement (a capite ad calcem), in part to the hot, dry, and dusty climate of Egypt that exacerbated ophthalmic maladies, and in part to the absence of powerful antiseptics that facilitated disease transmission, eye diseases were nonetheless conditions that medical practitioners of the Roman period were able to ameliorate with considerable success through their compound salves (collyria) and eyewashes. The auxiliary troops at Vindolanda suffering from eye disease (lippientes) most likely had their inflamed eyes and conjunctivitis treated with salves that arrived in camp in dried form, imprinted with a collyrium stamp explaining its precise use (Jackson 1988: 83-5). More than 300 collyrium stamps made of stone have survived from the northern provinces of Britain, Gaul, and Germany. In the warmer and drier climates bordering on the Mediterranean, the salves no doubt circulated in moist form in vials and jars. Directions for preparing eye salves and washes also dominated the papyri from Egypt that contained recipes, underscoring the likelihood that many in the populations of the Roman Empire suffered from ophthalmias and relied on such medicaments to ease them (Marganne 1994: 173-6; Andorlini 2001: 139-47). The medical definitions and questions-and-answer texts enjoyed empire-wide popularity, for not only do we find papyrus fragments of them in Greek-speaking Egypt throughout antiquity, but beginning in the tenth century ce copies on parchment appear in the west, now translated into Latin and not infrequently attributed to Soranus. The following excerpt from a Latin version paraphrased the Hippocratic Oath, manipulating it in a manner similar to Scribonius Largus’ discussion:
Let us, moreover examine what kind of man ought to be a doctor. He must be kindly in his habits and moderate with the expected honorable qualities, nor should a certain holiness be lacking to him, nor should he be haughty. He must give treatment equally to poor and rich, slave and free. Among doctors medicine is a unity. If indeed they are paid money, let them accept it and not refuse; but if pay is not forthcoming, let them not demand it, for however much a person has paid cannot be equated with the benefits medicine conveys. Into whatever homes the doctor enters, he must have before his eyes curing to the extent of his ability. Let him be mindful of the Oath of Hippocrates so that he hold himself off from all blame and especially from sexual and criminal acts, and what ever is said or done in the house he should conceal as he would a sacred mystery. As a result, he will acquire more abundant praise for himself and for his art. (Quaest. med., 245.10-20 Rose)
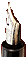

 World History
World History









